Varicose Vein Treatment Options for Healthier Legs
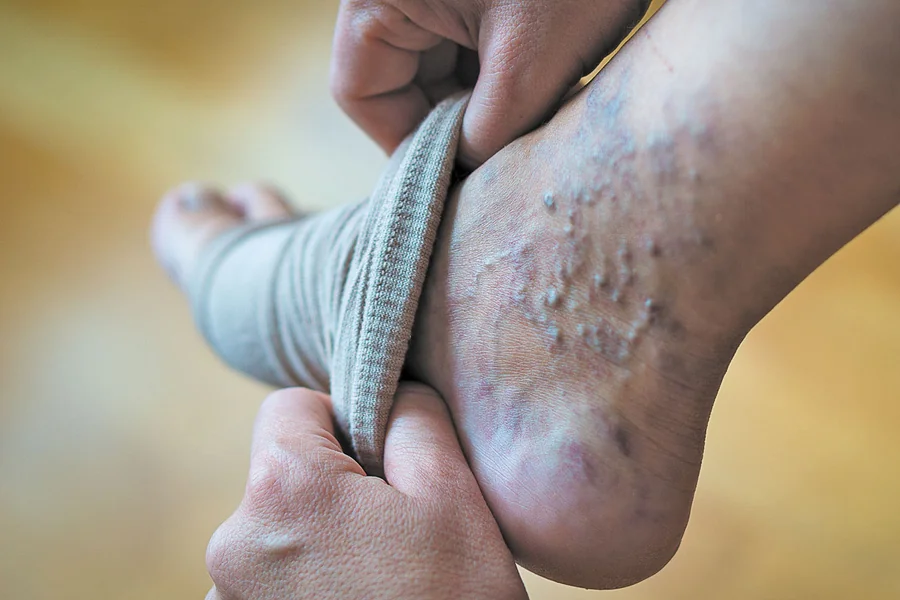
Varicose vein treatment options for healthier legs range from simple lifestyle changes to advanced procedures performed in modern outpatient settings. For busy professionals—such as online business owners, affiliate marketers, and SEO agency teams—leg pain, swelling, or visible bulging veins can interfere with productivity, travel, and daily comfort.
This guide explains what varicose veins are, when to seek medical evaluation, and which conservative care options can be started immediately. It also covers minimally invasive treatments designed to reduce downtime, as well as situations where vein surgery in Central Austin may be the most effective solution for long-term relief. Written with efficiency in mind, the article helps readers evaluate risks, recovery timelines, and costs so they can confidently choose the right next step for their vein health.
What are Varicose Veins? Causes, Symptoms, and Who’s at Risk
Varicose veins are dilated, tortuous veins usually visible just under the skin of the legs. They develop when one-way valves inside veins weaken, allowing blood to pool instead of moving efficiently back toward the heart. Over time, this pressure stretches the vein walls and makes veins appear blue or purple and rope-like.
Common symptoms include aching, heaviness, itching, visible bulging veins, and swelling that worsens toward the end of the day. Skin changes, discoloration, dryness, or ulceration signal more advanced disease.
Risk factors increase the likelihood of developing varicose veins. They include:
- Age: valve tissue weakens with time.
- Sex: women are affected more often, partly due to pregnancy and hormones.
- Family history: genetics plays a strong role.
- Prolonged standing or sitting: occupations that keep people immobile raise the risk.
- Obesity and lack of activity: both increase venous pressure.
For the site’s audience, people who travel for conferences, sit for long stretches writing content, or manage remote teams, the combination of prolonged sitting and irregular exercise can accelerate symptoms. Recognizing early signs helps avoid progression and limits lost time at work.
When to See a Doctor: Signs You Need Evaluation
Not every visible vein requires treatment, but a timely medical evaluation is important if symptoms interfere with daily life or indicate complications. One should seek care when:
- Pain, cramping, or leg heaviness limit activity or work productivity.
- Swelling persists even though elevation or during travel.
- Skin around the ankle darkens, becomes tight, or wounds develop.
- Veins bleed after minor trauma, or there’s sudden worsening of pain, warmth, or redness, possible signs of thrombophlebitis or deep vein thrombosis.
A clinician will perform a focused history and physical exam and typically order a duplex ultrasound to map the superficial and deep venous systems. Ultrasound results guide whether conservative measures will suffice or whether procedural treatment is warranted.
Conservative and Nonprocedural Options
Many people start with conservative strategies that reduce symptoms and may slow progression. These options are appropriate for mild disease, for those who prefer to avoid procedures, or as adjuncts after an intervention.
Compression Stockings: Types and Proper Use
Compression stockings remain the cornerstone of nonprocedural treatment. They apply graded pressure, highest at the ankle and decreasing up the leg, to assist venous return.
Types include:
- Over-the-counter support stockings (mild compression, 8–15 mmHg)
- Prescription-strength graduated compression (20–30 mmHg or 30–40 mmHg)
- Thigh-high, knee-high, and pantyhose styles
Proper use matters; stockings should be put on in the morning before swelling begins and removed before bed. They should fit snugly but not painfully. For people who travel or have intermittent symptoms, wearing them on long flights or standing days can prevent flare-ups.
Lifestyle Changes: Exercise, Weight Management, and Leg Care
Modifiable behaviors make a big difference. Regular walking or calf-strengthening exercises act as a “second heart” by pumping venous blood upward. Weight loss reduces venous pressure in the legs. Practical tips:
- Stand and stretch every 30–60 minutes during long work sessions.
- Add short walks between meetings or blocks of writing.
- Elevate legs above heart level for 15–20 minutes daily when possible.
- Avoid tight clothing around the groin and high heels on long days.
These measures are low-cost and support overall health, useful for entrepreneurs who prefer conservative, nonmedical options.
Medications and Topical Therapies: What They Can (and Can’t) Do
Oral venoactive drugs (like micronized flavonoids) and topical agents may reduce symptoms such as aching and swelling, but they don’t fix valve failure. They’re used adjunctively, often to control symptoms while awaiting a procedure or for those not suited to interventions. Over-the-counter pain relievers can help short-term: anti-inflammatory creams may ease local discomfort. Expect modest benefits and consult a clinician for guidance on specific products.
Minimally Invasive Procedures
Minimally invasive treatments have become first-line for symptomatic varicose veins because they offer high efficacy with shorter recovery than traditional surgery. Most procedures are performed under local anesthesia in outpatient settings.
Endovenous Thermal Ablation: Laser (EVLA) and Radiofrequency (RFA)
Endovenous laser ablation (EVLA) and radiofrequency ablation (RFA) use heat delivered inside the vein to collapse and seal the incompetent vein. They have advantages:
- Success rates above 90% for great saphenous vein reflux
- Minimal incisions and quick return to activity (often within a day or two)
- Low complication rates compared with open surgery
Patients may experience bruising, temporary numbness, or mild soreness. Compression stockings are usually recommended for a short period after treatment.
Ultrasound-Guided Foam and Liquid Sclerotherapy
Sclerotherapy involves injecting a solution or foam that irritates the vein lining, causing it to collapse and be reabsorbed. Ultrasound guidance allows treatment of deeper or larger veins. Sclerotherapy is ideal for smaller varicosities and cosmetic spider veins and is often combined with ablation for comprehensive care. Multiple sessions may be needed, and patients should avoid prolonged sun exposure after treatment: pigmentation changes can occur.
Ambulatory Phlebectomy for Surface Veins
Ambulatory phlebectomy removes superficial bulging veins through tiny skin punctures. It’s effective for large surface veins left behind after treating reflux or when surface bulges are the main concern. Recovery is typically quick, with localized bruising and short periods of compression.
Surgical Options and When They’re Recommended
Surgery is less common than in past decades but still appropriate in certain circumstances, especially when anatomy or prior treatments make minimally invasive options impractical.
Combination Procedures and When Surgery is Preferred
Complex cases may need a hybrid approach, ablation of the main refluxing vein combined with phlebectomy or sclerotherapy for tributaries. Surgery is also favored when previous interventions have failed or when deep venous disease requires open correction by a vascular surgeon. The decision is individualized based on duplex findings, patient health, and goals.
Recovery, Risks, and Expected Outcomes
Understanding recovery, potential complications, and expected outcomes helps patients plan time off, travel, and follow-up care.
Typical Recovery Timelines and Aftercare Tips
- Conservative care: immediate, ongoing management with symptom improvement in days to weeks.
- Ablation and sclerotherapy: most return to normal activity within 24–72 hours; avoid heavy lifting and prolonged standing for a few days.
- Phlebectomy and surgery: may require 1–2 weeks of reduced activity; full recovery varies by extent of procedure.
Aftercare commonly includes wearing compression stockings for a prescribed period, walking daily, and attending a follow-up ultrasound to confirm vein closure.
Potential Complications and How They’re Managed
Complications are uncommon but include:
- Bruising and localized pain
- Superficial thrombophlebitis or clot formation in treated veins
- Nerve injury causing numbness or tingling (often temporary)
- Skin discoloration or texture changes
Clinicians manage these with conservative measures, anti-inflammatory medication, compression, and occasionally anticoagulation or further procedural intervention.
How to Choose the Right Treatment: Questions to Ask Your Provider
Choosing a treatment involves matching goals (symptom relief vs. cosmetic improvement), anatomy, and lifestyle. Useful questions to ask:
- What does my duplex ultrasound show, and which veins are causing symptoms?
- What are the expected benefits and risks of each option for my anatomy?
- How much downtime should I plan, and when can I travel or return to work?
- What follow-up and recurrence rates can I expect?
- Will multiple sessions be needed, and what are the costs?
Clear answers help align expectations and minimize disruption for professionals juggling business commitments.
Cost, Insurance Considerations, and Access to Care
Costs vary by procedure, geographic region, and whether treatment is covered by insurance. Many insurers cover treatment when varicose veins cause documented symptoms or complications: purely cosmetic treatments may be denied. Key points for budgeting and access:
- Get a preauthorization from insurance when possible and a clear quote for out-of-pocket costs.
- Minimally invasive outpatient procedures often cost less than traditional surgery when factoring in recovery time and lost work.
- For those without easy access to vascular specialists, local interventional radiology or vein clinics provide many modern treatments; telehealth can be used for initial consultations.
Professionals managing business expenses should weigh the cost of treatment against lost productivity from ongoing symptoms. Investing in treatment often yields quicker functional recovery and less long-term disruption.
Conclusion
Varicose vein treatment options for healthier legs range from conservative measures that can be started immediately to minimally invasive procedures with rapid recovery, and, in select cases, traditional surgery. For people whose livelihoods depend on travel, long workdays, or consistent output, like SEO professionals and agency owners, addressing symptomatic varicose veins promptly reduces downtime and protects long-term leg health.
A duplex ultrasound is the pivotal diagnostic step that guides therapy. Patients should balance symptom severity, recovery tolerance, and cost when choosing treatment, and come prepared with targeted questions for their provider. With modern options, most people achieve meaningful symptom relief and improved leg appearance with minimal interruption to their professional lives.