When Revision Spine Surgery Is Needed After a Failed Back Procedure
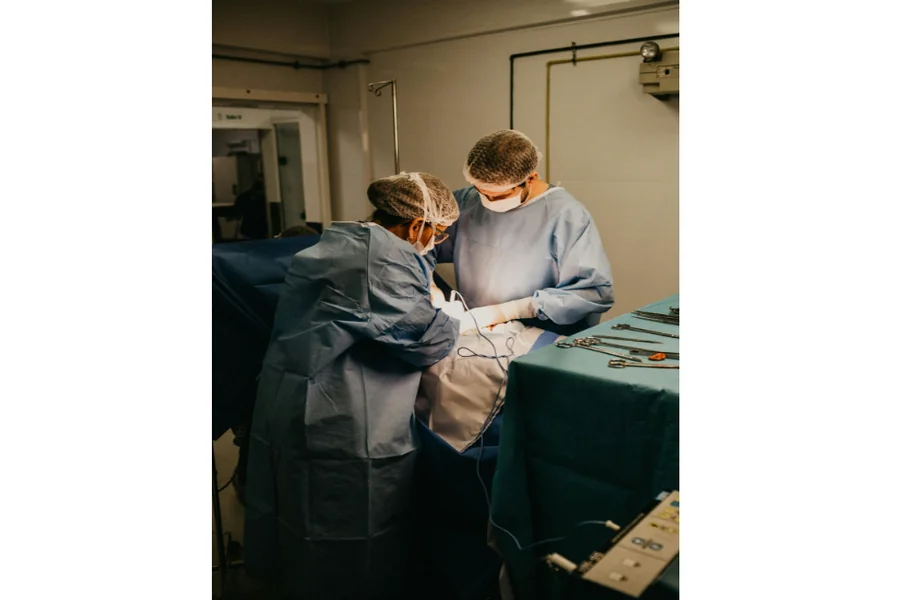
If you’ve undergone back surgery but still experience pain or new neurological symptoms, it may indicate that the initial procedure didn’t fully address the problem. Factors like scar tissue, nerve compression, or degeneration of nearby spinal segments can complicate recovery and require further intervention. Understanding when revision spine surgery is appropriate involves careful assessment and diagnostic imaging—critical steps before deciding on the next course of action.
Understanding the Causes of Failed Back Surgery
Although revision spine surgery aims to correct issues from the initial procedure, understanding why the original surgery failed is essential for planning your next steps. Failed back surgery can result from multiple factors, including surgical errors such as improper hardware placement, inadequate decompression, or failure to address the underlying pathology. These technical shortcomings may lead to persistent pain, neurological deficits, or spinal instability. For patients in need of specialized care, consulting providers who perform expert revision spinal procedures in New Jersey can help ensure a tailored and precise surgical plan. Additionally, mismatched patient expectations often contribute to dissatisfaction; if your anticipated outcomes were unrealistic or not clearly communicated, you might perceive the surgery as unsuccessful despite objective improvement. Other causes can include progression of degenerative disease or scar tissue formation causing nerve irritation. Accurately identifying these causes through thorough imaging and clinical evaluation enables your surgeon to minimize further risk and optimize your chances for a successful revision outcome.
Identifying Persistent or New Symptoms After Surgery
After your initial spine surgery, it’s essential to monitor for persistent pain that doesn’t improve or worsens, as this may indicate incomplete resolution or complications. You should also be alert for any new neurological symptoms, such as numbness, weakness, or changes in bladder or bowel function, which could signal nerve involvement. Early identification of these signs helps guide timely evaluation and potential revision surgery.
Recognizing Ongoing Pain
When you experience persistent or new pain following spine surgery, it is crucial to distinguish between normal postoperative discomfort and symptoms indicating surgical failure or complications. Normal recovery pain typically decreases steadily within weeks, whereas chronic discomfort that intensifies or fails to improve may signal unresolved issues such as scar tissue formation, hardware failure, or nerve irritation. Accurate recognition of ongoing pain involves thorough clinical evaluation and imaging studies to identify structural causes. Effective pain management during this phase is critical to maintaining function and quality of life. If conservative measures fail and symptoms persist, revision surgery might be necessary to address the underlying pathology. Monitoring pain patterns closely helps you and your surgeon determine whether the pain reflects a manageable postoperative phase or a complication requiring intervention.
Detecting New Neurological Issues
Persistent or worsening pain after spine surgery may be accompanied by new neurological symptoms that indicate nerve involvement or damage. It’s essential you undergo a thorough neurological assessment to detect these issues early. During symptom evaluation, focus on identifying changes that suggest nerve compromise. Key indicators include:
- Numbness or tingling sensations in the limbs, which may signal nerve irritation.
- Muscle weakness or loss of motor function, indicating potential nerve root compression.
- Altered reflexes, which can reveal nerve pathway disruptions.
- New onset bowel or bladder dysfunction, a serious sign requiring immediate attention.
Promptly reporting these symptoms to your surgeon allows for timely intervention, potentially preventing further nerve damage and improving surgical outcomes.
Common Complications Leading to Revision Spine Surgery
When you face persistent pain after a back procedure, it often signals unresolved issues like nerve compression or scar tissue formation. Hardware malfunction, such as screw loosening or rod breakage, is another common complication requiring revision. Understanding these factors is essential for planning effective corrective surgery.
Persistent Pain Sources
Although revision spine surgery aims to address previous surgical failures, you should recognize that ongoing pain often stems from specific, identifiable complications. Understanding these persistent pain sources is essential for effective pain management strategies and utilizing patient education resources. Common causes include:
- Epidural fibrosis causing nerve root tethering and irritation.
- Recurrent disc herniation leading to renewed nerve compression.
- Adjacent segment degeneration resulting in instability and pain.
- Incomplete decompression leaving residual nerve impingement.
Each of these factors can contribute to continued discomfort despite initial surgery. By identifying the exact source, you can better tailor interventions, whether surgical or conservative. Incorporating thorough patient education resources helps set realistic expectations and optimizes pain management strategies, ultimately improving outcomes and reducing the likelihood of further revision procedures.
Hardware Malfunction Issues
Beyond ongoing pain sources like epidural fibrosis or recurrent herniation, hardware malfunction represents a significant cause of failure requiring revision spine surgery. When the implanted devices—such as rods, screws, or plates—lose hardware stability due to loosening, breakage, or migration, it compromises spinal alignment and function. You may experience renewed pain, neurological symptoms, or structural instability. These issues often stem from biomechanical stress, suboptimal surgical techniques, or patient factors like osteoporosis. During revision surgery, your surgeon must carefully assess hardware integrity through imaging and intraoperative evaluation. The goal is to restore hardware stability by replacing or reinforcing the implants, often employing advanced surgical techniques tailored to your anatomy and pathology. Addressing hardware malfunction promptly is critical to prevent further complications and to improve surgical outcomes.
Diagnostic Tools Used to Evaluate Post-Surgical Spine Issues
Since spinal anatomy can be markedly altered after surgery, accurately diagnosing post-surgical complications requires a combination of advanced imaging modalities and clinical assessments. Thanks to imaging advancements, your physician can achieve greater diagnostic accuracy when evaluating complex post-operative changes. Here are key diagnostic tools used:
- Magnetic Resonance Imaging (MRI): Provides detailed soft tissue contrast, essential for detecting nerve compression, scar tissue, or recurrent disc herniation without radiation exposure.
- Computed Tomography (CT) Scan: Offers high-resolution bone imaging to assess hardware position, fusion status, and osseous abnormalities.
- X-rays (Dynamic and Static): Useful for evaluating spinal alignment, hardware integrity, and instability under movement.
- Electromyography (EMG) and Nerve Conduction Studies (NCS): Help identify nerve root dysfunction and differentiate neuropathic from mechanical causes of pain.
Using these precise tools together enhances your doctor’s ability to pinpoint the cause of persistent symptoms following spine surgery.
Assessing Patient Eligibility for Revision Spine Surgery
To determine if you’re a candidate for revision spine surgery, a thorough evaluation of your medical history is essential to identify any underlying conditions or previous complications. Advanced imaging and diagnostic tests will be used to assess the current state of your spine and pinpoint the cause of persistent symptoms. This combined approach guarantees that the surgical risks and potential benefits are accurately weighed before proceeding.
Medical History Evaluation
Although imaging and physical examination provide critical information, a thorough medical history evaluation is essential in determining your eligibility for revision spine surgery. Your patient background and detailed surgical history offer crucial clues regarding potential risks and expected outcomes. During this evaluation, the surgeon will:
- Review previous spine surgeries, noting techniques and complications.
- Assess comorbidities such as diabetes or osteoporosis that may impair healing.
- Evaluate medication use, including anticoagulants and pain management regimens.
- Identify any history of infection or neurological deficits related to prior procedures.
This extensive history guides the surgical team in tailoring the revision approach, anticipating challenges, and optimizing your safety. Accurate documentation helps distinguish between surgical failure and other causes of persistent symptoms, ensuring revision surgery is appropriate and timely.
Imaging and Diagnostics
When evaluating your eligibility for revision spine surgery, imaging and diagnostic tests play a critical role in identifying anatomical changes, hardware status, and sources of persistent symptoms. Advanced imaging techniques such as MRI, CT scans, and dynamic X-rays provide detailed visualization of soft tissue, bony structures, and implant positioning. These modalities help determine if issues like adjacent segment degeneration, pseudarthrosis, or hardware failure are present. Diagnostic accuracy is enhanced by combining imaging findings with clinical evaluations, including nerve conduction studies when radiculopathy is suspected. Accurate interpretation of these tests guides surgical planning, ensuring revision surgery targets the specific pathological issues causing your symptoms. Ultimately, precise imaging and diagnostics are indispensable for determining whether you’re a suitable candidate for revision surgery, minimizing risks, and optimizing outcomes.
Surgical Techniques Used in Revision Procedures
Mastering surgical techniques in revision spine surgery is essential because these procedures often involve complex anatomy altered by previous interventions. When you approach revision surgery, you’ll often rely on:
- Minimally invasive techniques – These reduce tissue disruption and scar formation, facilitating faster recovery and less postoperative pain.
- Fusion options – Choosing between anterior, posterior, or lateral fusion approaches depends on the prior surgery and current pathology.
- Decompression methods – Tailored to relieve nerve impingement while preserving stability, often requiring meticulous scar tissue dissection.
- Instrumentation strategies – Revision cases may necessitate customized hardware placement to accommodate altered bone structure and previous implants.
Risks and Challenges Associated With Revision Spine Surgery
Since revision spine surgery involves operating on previously altered anatomy, you face increased risks compared to primary procedures. Scar tissue, altered landmarks, and changes in spinal biomechanics complicate the surgical approach, raising the likelihood of surgical complications such as dural tears, nerve injury, and infection. These factors demand meticulous preoperative planning and intraoperative navigation to minimize adverse events.
Additionally, surgical time may be prolonged, and blood loss can be greater, increasing perioperative risk. You might also experience heightened patient anxiety due to the complexity and uncertainty surrounding revision surgery outcomes. Addressing this anxiety through clear communication and realistic expectations is essential for informed consent and postoperative compliance.
Understanding these risks helps you weigh the benefits of revision surgery against potential challenges. Your surgeon’s expertise in handling altered spinal anatomy and anticipating complications plays a significant role in optimizing safety and effectiveness during your revision spine procedure.
Recovery Expectations and Rehabilitation After Revision Surgery
Although revision spine surgery can address persistent or recurrent issues, your recovery process is often more complex and prolonged than after a primary procedure. Understanding rehabilitation protocols and realistic recovery timelines is essential for ideal outcomes. Here’s what you should expect:
- Extended Recovery Timelines: Healing can take several months longer due to scar tissue and altered anatomy from previous surgeries.
- Customized Rehabilitation Protocols: Physical therapy will be tailored to your specific surgical intervention and functional limitations, focusing on gradual mobility restoration and strength building.
- Pain Management Complexity: You may require more intensive pain control strategies as nerves and tissues have been previously disturbed.
- Close Monitoring: Frequent follow-ups are essential to assess healing progress and promptly address complications such as infection or hardware issues.
Non-Surgical Alternatives to Consider Before Revision
Before opting for revision spine surgery, you should thoroughly explore non-surgical alternatives that might alleviate your symptoms or improve function. Alternative therapies such as physical therapy, chiropractic care, and targeted pain management techniques can address underlying muscular imbalances and nerve irritation without invasive intervention. Additionally, modalities like acupuncture or transcutaneous electrical nerve stimulation (TENS) may provide symptomatic relief.
Lifestyle modifications also play an important role. Implementing ergonomic adjustments, weight management, and tailored exercise regimens can reduce mechanical stress on your spine and enhance stability. Avoiding activities that exacerbate pain while adopting core-strengthening routines may improve long-term outcomes.
Evaluating these options under the guidance of a multidisciplinary team guarantees a thorough approach. Only after exhausting or determining the insufficiency of these non-surgical measures should revision surgery be considered. This strategy minimizes surgical risks while optimizing your chances for meaningful symptom improvement.
Long-Term Outcomes and Success Rates of Revision Spine Surgery
Understanding the long-term outcomes and success rates of revision spine surgery is critical when weighing your treatment options after a failed back procedure. Success rates can vary due to factors such as the complexity of the initial surgery and underlying pathology. Here’s what you need to reflect on about long term outcomes:
- Revision surgeries generally show lower success rates than primary procedures, with reported improvement in pain and function ranging from 50% to 75%.
- Long term outcomes greatly depend on accurate diagnosis of the cause of failure, such as persistent nerve compression or spinal instability.
- Complication rates tend to be higher in revision cases, affecting overall success and recovery trajectory.
- Patient-specific factors, including overall health and adherence to rehabilitation, greatly influence sustained improvements post-surgery.
Frequently Asked Questions
How Much Does Revision Spine Surgery Typically Cost?
Revision spine surgery typically costs between $50,000 and $150,000. Cost factors include hospital fees, surgeon expertise, and complexity. You should explore financial assistance options, like insurance coverage or payment plans, to manage expenses effectively.
Will Insurance Usually Cover Revision Spine Surgery?
Insurance policies often cover revision spine surgery, but coverage criteria vary considerably. You’ll need to verify if your insurer requires documented medical necessity, previous treatment failure, and pre-authorization before approving the procedure and related costs.
How Do Surgeons Decide on the Timing for Revision Surgery?
Surgeons determine surgical timing considerations by evaluating your patient recovery factors, symptom progression, and imaging results. They balance ideal healing from prior surgery with the urgency of symptoms, ensuring revision surgery is scheduled when benefits outweigh risks.
Can Lifestyle Changes Prevent the Need for Revision Surgery?
Yes, adopting lifestyle changes like regular exercise benefits spinal health and supports weight management, reducing stress on your spine. These measures can decrease complications, potentially preventing the need for revision surgery by enhancing overall recovery and stability.
What Are the Signs That Revision Surgery Should Be Avoided?
You should avoid revision surgery if warning signs like severe infection, poor bone quality, or uncontrolled comorbidities appear. A thorough patient evaluation is essential to identify these factors and determine if surgery risks outweigh benefits.