Dental Restoration Options: A Comprehensive Review of Modern Techniques
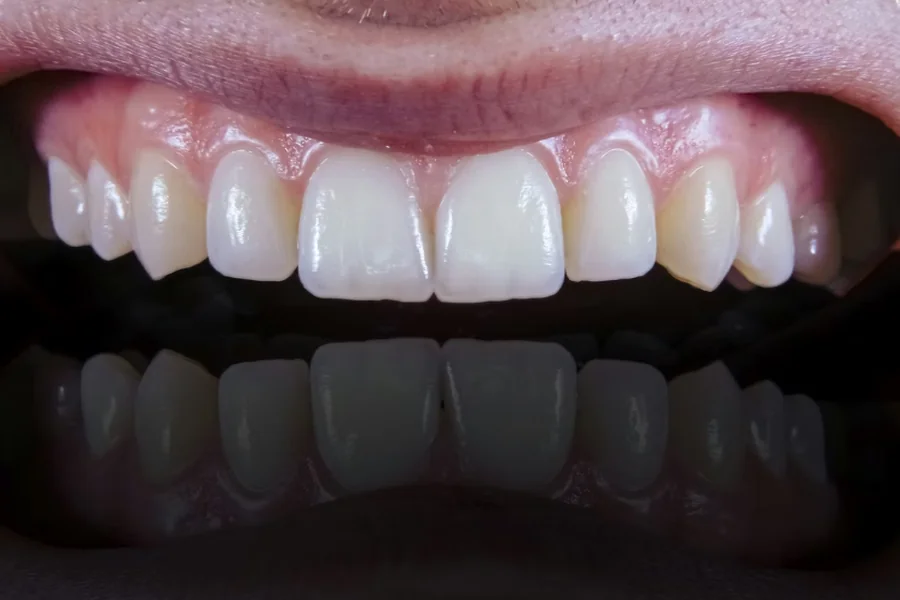
Every year, nearly 178 million Americans lose at least one tooth, and by age 65, approximately 26% have lost all their permanent teeth according to the American College of Prosthodontists. These numbers represent more than statistics—they reflect millions of people facing decisions about how to restore their oral health, function, and confidence. What’s particularly striking is that modern dentistry now offers more sophisticated restoration options than ever before, yet many patients remain unaware of the full spectrum of possibilities available to them.
The landscape of dental restoration has transformed dramatically over the past decade. Digital dentistry, biocompatible materials, and minimally invasive techniques have revolutionized how dentists approach tooth restoration. Where patients once faced limited choices—often between basic fillings or full tooth extraction—today’s dental restoration options span a sophisticated range of materials, techniques, and outcomes tailored to individual needs, oral health conditions, and long-term functional goals.
Understanding these options matters because the choice you make about dental restoration affects not just your immediate comfort, but your long-term oral health, functionality, and quality of life. The wrong choice can lead to repeated procedures, higher costs, and compromised outcomes. Here’s what current research and clinical practice reveal about navigating today’s dental restoration landscape effectively.
What Are Dental Restoration Options?
Dental restoration encompasses any treatment designed to repair, replace, or enhance damaged, decayed, or missing teeth. Unlike cosmetic dentistry, which focuses primarily on appearance, restorative dentistry prioritizes function while simultaneously addressing aesthetic concerns. The fundamental goal is restoring your teeth’s structural integrity, chewing function, and protective capacity against further decay or damage.
Who needs dental restorations? The answer is broader than many people realize. Beyond obvious cases like cavities or broken teeth, restorations address worn enamel from grinding, failed previous dental work, genetic tooth defects, and age-related deterioration. According to the National Institute of Dental and Craniofacial Research, 92% of adults aged 20-64 have had dental caries in their permanent teeth—meaning nearly everyone will eventually need some form of restoration.
The scope of restoration options has expanded significantly with technological advances. Modern restorative dentistry can address everything from minor surface defects to complete smile reconstruction. Materials science has introduced ceramics that match natural tooth translucency, composites that bond molecularly with tooth structure, and implant systems with 95%+ success rates over 10-15 years.
What sets contemporary restoration apart is the emphasis on conservative treatment—preserving as much natural tooth structure as possible while achieving optimal function and longevity. This philosophy has shifted the field away from the “drill and fill” mentality toward precision techniques that maintain tooth vitality whenever feasible.
How Do Dental Restorations Work?
Common Procedures and Their Steps
Understanding restoration mechanics helps patients make informed decisions about their treatment. Most restorative procedures follow a similar pattern: assessment, preparation, restoration placement, and follow-up care. However, the specifics vary dramatically based on the extent of damage and chosen treatment approach.
Direct restorations like composite fillings happen chairside in a single appointment. The dentist removes decayed material, applies bonding agents that create molecular adhesion with tooth structure, then layers composite material that’s light-cured to hardness. The restoration is shaped and polished to match natural tooth contours. Success depends heavily on moisture control and precise technique during placement.
Indirect restorations require multiple appointments and laboratory fabrication. Crowns, bridges, and complex inlays involve tooth preparation, impression taking (digital or traditional), temporary restoration placement, then final restoration fitting and cementation. Digital workflows using CAD/CAM technology can sometimes compress this timeline, with some offices offering same-day ceramic restorations.
Implant-based restorations represent the most complex category, involving surgical placement of titanium posts into jawbone, healing periods for osseointegration (bone fusion), and finally crown attachment. The entire process typically spans 3-6 months, though immediate loading protocols exist for specific cases.
Materials Used in Dental Restorations
Material selection profoundly impacts restoration longevity, function, and aesthetics. Each material category offers distinct advantages and limitations that affect treatment outcomes.
Ceramic materials dominate high-end restorations due to their biocompatibility and aesthetic properties. Lithium disilicate ceramics like IPS e.max provide excellent translucency matching natural enamel, while zirconia offers superior strength for posterior restorations handling high chewing forces. Research published in the Journal of Prosthodontic Research shows 10-year survival rates exceeding 90% for well-executed ceramic restorations.
Composite resins have evolved beyond simple cavity fillings to include complex smile makeovers. Modern nano-filled composites resist wear and staining while providing excellent color matching. However, they require periodic replacement—typically every 7-12 years depending on location and patient factors like grinding or diet.
Metal alloys still play crucial roles, particularly in implant systems where titanium’s biocompatibility enables osseointegration. Gold alloys, while less popular aesthetically, offer unmatched longevity for posterior restorations, with documented cases lasting 30+ years. The trade-off involves appearance and higher material costs.
Bioactive materials represent an emerging category that actively promotes tooth remineralization. Glass ionomer cements release fluoride over time, while newer bioactive composites attempt to recreate some of natural tooth structure’s self-repair capabilities.
Types and Variations of Dental Restorations
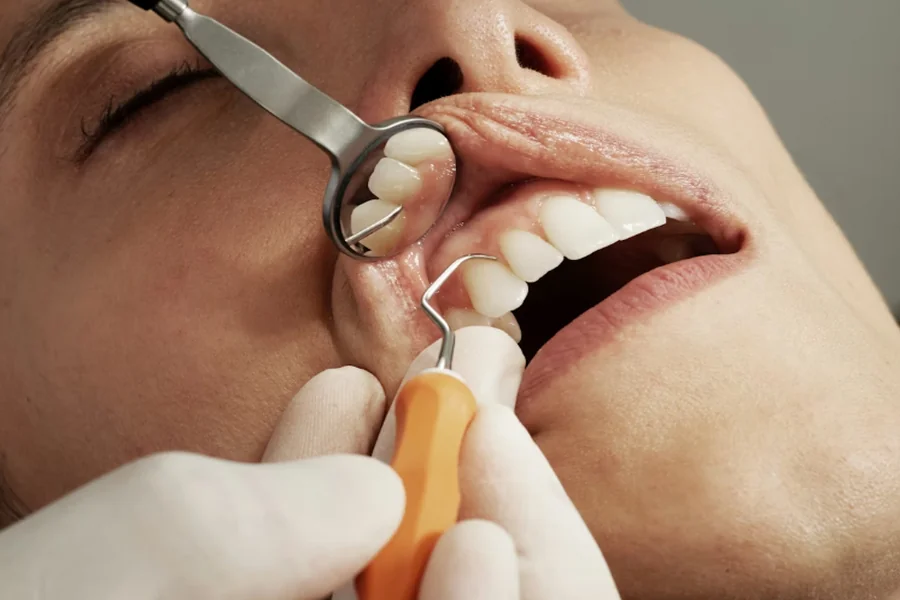
Modern dental restoration encompasses seven primary categories, each addressing specific clinical situations and patient needs. Understanding their applications helps clarify which options might suit your particular circumstances.
Composite fillings handle cavities and minor tooth damage through direct placement of tooth-colored resin materials. They work well for front teeth and smaller posterior cavities, offering immediate results and conservative tooth preparation. Limitations include gradual wear under heavy chewing forces and potential staining over time.
Crowns completely cover damaged teeth when decay or fracture has compromised structural integrity. Whether ceramic, metal, or combination materials, crowns restore full function while protecting remaining tooth structure. They’re particularly valuable after root canal therapy when teeth become more brittle and prone to fracture.
Dental bridges replace one or more missing teeth by anchoring artificial teeth to adjacent natural teeth or implants. Traditional bridges require crowning adjacent teeth, while implant-supported bridges preserve neighboring teeth. Success rates vary based on span length and supporting tooth health.
Dental implants represent the gold standard for single tooth replacement, providing independent support that doesn’t compromise adjacent teeth. Titanium posts integrate with jawbone, supporting crowns, bridges, or dentures. While requiring surgical procedures and healing time, implants offer the most natural function and longest-term value.
Inlays and onlays address moderate damage between simple fillings and full crowns. These lab-fabricated restorations preserve healthy tooth structure while providing superior strength compared to large fillings. They’re particularly effective for cuspal damage or large cavities in posterior teeth.
Dentures—both partial and complete—address multiple missing teeth when implants aren’t feasible. Modern denture materials and attachment systems have dramatically improved retention and comfort, though they still require adjustment periods and periodic maintenance.
Composite bonding repairs chips, gaps, and surface defects through direct application of tooth-colored materials. It’s minimally invasive and reversible, making it ideal for minor aesthetic improvements and small restorations.
How Do Dental Restoration Options Compare?
Durability varies significantly among restoration types based on materials, placement techniques, and patient factors. Clinical research provides clear guidance on expected lifespans, though individual results depend on oral hygiene, diet, grinding habits, and professional maintenance.
Longevity rankings show interesting patterns. Implant-supported single crowns demonstrate 95-98% survival rates at 10 years, making them the most durable option for single tooth replacement. Well-executed ceramic crowns achieve 85-95% survival at 10 years, while large composite fillings typically require replacement every 7-12 years. Bridges show variable outcomes depending on span length and abutment tooth health.
Functional considerations reveal trade-offs between restoration types. Implants provide the most natural chewing force distribution, allowing patients to eat virtually anything. Fixed bridges restore significant function but may create cleaning challenges around pontic areas. Removable partial dentures offer reasonable function but limit diet choices due to retention concerns.
Maintenance requirements differ substantially. Implant-supported restorations require standard brushing and flossing with some attention to gum health around implant sites. Bridges demand specialized flossing techniques and possible water flosser use. Dentures require daily removal, cleaning, and periodic adjustments as tissues change over time.
Cost-effectiveness extends beyond initial treatment fees. While implants carry higher upfront costs, their longevity and minimal maintenance often provide better long-term value compared to repeatedly replacing less durable options. Composite fillings offer immediate affordability but may require more frequent replacement. Insurance coverage varies significantly among restoration types, with basic fillings typically covered while cosmetic improvements often aren’t.
The comparison isn’t simply about “best” versus “worst” options—it’s about matching restoration characteristics to individual circumstances, expectations, and long-term goals.
What Are the Outcomes and Patient Experiences?
Success rates in dental restoration depend on multiple factors beyond the procedure itself. Patient selection, practitioner skill, material quality, and post-treatment care all influence outcomes. Understanding realistic expectations helps patients make informed decisions and achieve optimal results.
Success metrics vary by restoration type. For implants, success means osseointegration without mobility, infection, or persistent pain. Crown success involves maintaining proper fit, function, and absence of decay at margins. Composite restorations succeed when they maintain integrity without fracture, excessive wear, or secondary decay. According to systematic reviews published in Clinical Oral Implants Research, implant success rates consistently exceed 95% when proper protocols are followed.
Patient satisfaction correlates strongly with realistic expectations and adequate preparation. Studies show highest satisfaction among patients who understand treatment timelines, limitations, and maintenance requirements before beginning treatment. Dissatisfaction often stems from unrealistic expectations about immediate results, particularly with implant treatments requiring healing periods.
Common complications include temporary sensitivity after composite placement, margin discrepancies in crown work, and implant integration failures in compromised bone. Most complications are manageable when identified early through regular professional monitoring. Serious complications like nerve damage or severe infections remain rare—less than 2% in most published studies.
Risk factors significantly influence outcomes. Grinding or clenching (bruxism) can cause premature restoration failure, particularly with ceramic materials. Poor oral hygiene leads to decay around restoration margins and gum disease affecting supporting structures. Medical conditions like diabetes or osteoporosis may complicate healing, especially with surgical procedures.
Recovery experiences vary considerably. Simple composite fillings typically involve minimal discomfort and immediate return to normal function. Crown preparations may cause temporary sensitivity that resolves within days to weeks. Implant placement involves surgical recovery with swelling and discomfort lasting several days, followed by months of healing before final restoration placement.
The most successful restoration outcomes occur when patients actively participate in treatment planning, follow post-treatment instructions carefully, and maintain consistent professional care relationships.
What Are Current Trends and Future Developments?
Dental restoration continues evolving rapidly, driven by materials science advances, digital technology integration, and growing emphasis on minimally invasive techniques. Understanding these trends helps patients access the most current treatment options and prepare for future possibilities.
Digital dentistry has transformed restoration workflows from analog to digital processes. Intraoral scanners eliminate traditional impression materials, improving patient comfort while increasing accuracy. CAD/CAM systems enable same-day restorations in many cases, reducing appointment time and temporary restoration needs. 3D printing allows custom surgical guides and temporary restorations, improving precision and efficiency.
Bioactive materials represent a significant shift toward restorations that actively promote oral health. Newer composites release fluoride and other beneficial ions while some experimental materials attempt to stimulate natural tooth remineralization. Research from institutions like the University of Michigan suggests future restorations may actively prevent secondary decay rather than simply filling defects.
Minimally invasive protocols emphasize preserving healthy tooth structure through conservative preparation techniques. Laser technology enables precise tissue removal with minimal trauma. Air abrasion systems clean cavities without traditional drilling in some cases. These approaches reduce patient discomfort while maintaining more natural tooth strength.
Guided implant surgery uses CT imaging and computer planning to precisely position implants with minimal tissue trauma. Some protocols enable immediate implant placement and loading, dramatically reducing treatment time. Success rates with guided surgery often exceed traditional techniques while improving patient comfort.
Best practices emerging from current research emphasize comprehensive treatment planning that considers long-term oral health goals rather than isolated problem-solving. Interdisciplinary approaches combining periodontics, orthodontics, and restorative dentistry achieve more predictable and aesthetic outcomes. Patient education and shared decision-making have become integral to successful treatment.
The trend toward personalized dentistry means future restorations will increasingly account for individual genetic factors, oral microbiome characteristics, and lifestyle factors in treatment planning and material selection.
Common Questions and Misconceptions About Dental Restorations
Several persistent misconceptions about dental restoration can lead patients to delay necessary treatment or make suboptimal decisions. Addressing these misunderstandings helps patients navigate treatment options more effectively.
“Dental restorations always look artificial” represents perhaps the most common misconception. Modern ceramic materials and color-matching techniques achieve remarkable natural appearance. Digital shade analysis and characterization techniques help technicians recreate natural tooth translucency, surface texture, and color variations. Well-executed restorations should be virtually indistinguishable from natural teeth.
“Root canals always fail eventually” overlooks substantial improvements in endodontic techniques and success rates. Current research shows 85-95% success rates for properly executed root canal therapy, with many treatments lasting decades. Failure rates correlate more with delays in treatment, incomplete therapy, or inadequate coronal restoration than with inherent procedure limitations.
“Implants are only for elderly patients” ignores their value for younger patients with missing teeth. Age considerations focus on completed jaw development rather than maximum age limits. Healthy patients in their twenties through nineties can be excellent implant candidates when adequate bone and good oral hygiene exist.
“Composite fillings don’t last as long as silver fillings” reflects outdated information about older composite materials. Modern nano-filled composites demonstrate significantly improved wear resistance and longevity compared to early formulations. While amalgam fillings may last longer in some situations, composite materials offer superior aesthetics and more conservative tooth preparation.
Recovery expectations often unrealistic center around immediate perfect function and comfort. Most restorations require adaptation periods ranging from days to weeks as patients adjust to slightly different bite relationships or surface textures. Temporary sensitivity, especially with bonded restorations, typically resolves as teeth adapt to new materials and oral conditions normalize.
Understanding these realities helps patients approach dental restoration with appropriate expectations and greater confidence in treatment decisions. The key lies in open communication with dental professionals about concerns, expectations, and long-term oral health goals.
Final Thought
Modern dental restoration offers unprecedented opportunities to restore oral health, function, and aesthetics through sophisticated materials and techniques. The evolution from basic “drill and fill” dentistry to today’s precision, biocompatible approaches means patients can achieve outcomes that were impossible just decades ago. Success depends largely on matching appropriate restoration types to individual circumstances, understanding realistic timelines and expectations, and maintaining consistent professional care relationships.
As digital technology, bioactive materials, and minimally invasive techniques continue advancing, dental restoration will become even more predictable, comfortable, and durable. The organizations and practitioners leading this evolution focus not just on fixing immediate problems, but on comprehensive approaches that support long-term oral health and patient satisfaction. For patients facing restoration decisions today, the future has never looked more promising—or more personalized to individual needs and goals.