How Dental Crowns Restore Damaged Teeth for Lasting Smiles
Over 15 million dental crowns are placed annually in the United States, making crown restoration one of the most common procedures in modern dentistry. Yet despite their prevalence, many patients face crown-related complications within five years—often due to material selection or procedural factors that could have been addressed upfront. The stakes are significant: a failed crown doesn’t just mean another dental visit, it can compromise the underlying tooth structure and lead to more extensive treatments like root canals or extractions. For those seeking guidance on proper care and placement, Pittsburgh dental crown treatment can help ensure long-lasting results.
What’s driving the surge in crown procedures isn’t just an aging population. Modern lifestyles—from teeth grinding due to stress to dietary habits that accelerate enamel wear—are creating crown candidates at younger ages than ever before. Meanwhile, advances in dental materials and digital fabrication are revolutionizing how crowns are designed and placed, offering patients options that weren’t available even five years ago.
Understanding your crown options matters because this isn’t a one-size-fits-all solution. The material you choose, the preparation technique your dentist uses, and even the laboratory that fabricates your crown all impact both immediate comfort and long-term success. Here’s what current research and clinical practice reveal about making crown restoration work for the long term.
What Are Dental Crowns and Why Are They Used?
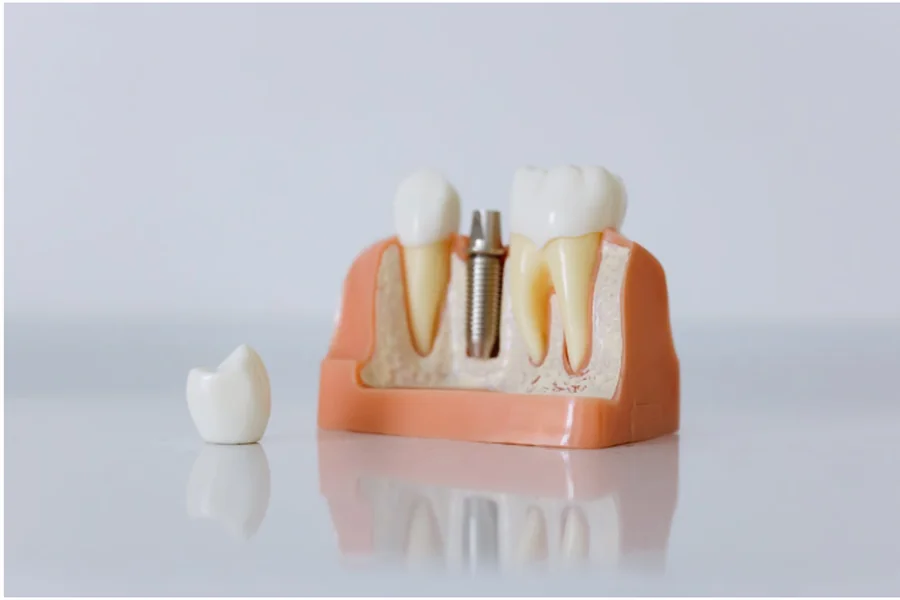
A dental crown functions as a protective cap that completely encases a damaged tooth, restoring both its shape and strength while preserving the natural tooth structure underneath. Think of it as architectural reinforcement—when a building’s facade becomes compromised, you don’t tear down the entire structure; you add protective cladding that restores both function and appearance.
Dentists recommend crowns when a tooth has sustained damage that goes beyond what a filling can address. This typically happens in several scenarios: after significant decay has removed substantial tooth structure, following root canal therapy where the tooth becomes brittle, when a tooth has cracked or fractured, or when previous large fillings have failed and weakened the remaining enamel. Unlike fillings that simply patch holes, crowns redistribute chewing forces across the entire tooth surface, preventing further breakdown.
The clinical goal extends beyond mere protection. Modern crown therapy aims to restore proper bite alignment, maintain facial support, and achieve natural aesthetics that blend seamlessly with surrounding teeth. When a back tooth loses structure, for instance, the opposing teeth can begin to over-erupt, leading to bite problems that affect the entire jaw system. A properly placed crown prevents this cascade of complications while returning the tooth to full function.
What makes crowns particularly valuable is their ability to address multiple problems simultaneously. A tooth weakened by decay regains strength, while discoloration or poor shape gets corrected through the crown’s exterior surface. This comprehensive approach explains why crowns often become the treatment of choice when patients want both functional restoration and cosmetic improvement in a single procedure.
How Do Dental Crowns Restore and Protect Teeth?
The restoration process begins with strategic removal of damaged tooth structure while preserving as much healthy tissue as possible. Your dentist carefully shapes the tooth to create an optimal foundation—removing decay and weakened areas while establishing the proper taper and height needed for crown retention. This preparation typically reduces the tooth’s dimensions by 1-2 millimeters on all surfaces, creating space for the crown material while maintaining structural integrity of the remaining tooth core.
Tooth Preparation and Impression Taking
Tooth shaping follows specific engineering principles that ensure long-term crown stability. The preparation must achieve adequate reduction for material thickness while maintaining enough tooth structure for retention. Dentists create a slight taper (typically 6-12 degrees) that allows the crown to seat properly without being too loose or too tight. Sharp angles are rounded to prevent stress concentrations that could lead to crown fracture, while the margin—where crown meets tooth—is carefully refined to ensure a precise seal.
Modern impression techniques have evolved significantly beyond the traditional putty molds that many patients remember. Digital scanning systems capture tooth dimensions with micron-level accuracy, creating 3D models that eliminate many variables associated with conventional impressions. These intraoral scanners use structured light or laser technology to map the prepared tooth, adjacent teeth, and bite relationship in real-time, often completing the process in under five minutes.
The digital workflow offers several advantages over conventional methods. Immediate verification ensures accuracy before the patient leaves the chair, while electronic transmission to dental laboratories speeds fabrication timelines. Perhaps most importantly, digital impressions capture fine details that affect crown fit—subtle undercuts, margin definition, and tissue contours that influence both retention and gum health around the finished restoration.
Fitting, Cementation, and Temporary Crowns
Temporary crowns serve a critical protective function during the fabrication period, typically lasting 1-3 weeks between appointments. These provisional restorations maintain tooth position, protect sensitive tooth structure from temperature changes and bacterial infiltration, and preserve gum contours around the preparation. Modern temporary materials—usually composite resin or acrylic—can be fabricated chairside in minutes, providing both function and reasonable aesthetics during the interim period.
When your permanent crown arrives from the laboratory, the fitting process involves several critical adjustments. Your dentist checks the crown’s fit against the prepared tooth, verifying that margins seat completely and contact points with adjacent teeth feel natural. Bite adjustment ensures that chewing forces distribute evenly without creating high spots that could cause discomfort or crown fracture. The internal surface may require minor modifications to achieve proper seating, while external contours are refined for optimal aesthetics and cleanability.
Cementation represents the final critical step that determines long-term success. Modern dental cements create both mechanical retention and chemical bonding between crown and tooth. The choice of cement depends on crown material—resin cements for ceramic crowns provide superior aesthetics and bonding strength, while glass ionomer or zinc phosphate cements offer reliable retention for metal-based restorations. Proper isolation during cementation prevents moisture contamination that could compromise the bond, while complete removal of excess cement prevents gum irritation and secondary decay.
Types and Materials of Dental Crowns
Crown selection has evolved from a simple choice between gold and porcelain to a sophisticated decision matrix involving aesthetics, strength, biocompatibility, and fabrication method. Each material category offers distinct advantages that make them optimal for specific clinical situations, patient preferences, and long-term expectations.
Metal and Porcelain-Fused-to-Metal Crowns
Metal crowns, particularly those made from gold alloys, remain the gold standard for durability in posterior applications. Gold’s unique properties—high corrosion resistance, excellent biocompatibility, and wear characteristics that match natural enamel—make it ideal for patients who prioritize longevity over aesthetics. Clinical studies show gold crowns lasting 15-20 years with proper care, significantly longer than most other materials. However, their obvious metallic appearance limits use to back teeth where aesthetics are less critical.
Porcelain-fused-to-metal (PFM) crowns attempt to combine metal’s strength with porcelain’s aesthetics by layering ceramic over a metal substructure. The metal core provides structural support while the porcelain veneer delivers tooth-like appearance. This hybrid approach dominated crown therapy for decades, offering a reasonable compromise between durability and cosmetics. PFM crowns typically last 10-15 years and remain cost-effective for many patients.
The limitation of PFM crowns lies in their aesthetic compromise. The underlying metal can create a gray line at the gum margin as gums naturally recede with age, while the porcelain layer can chip or fracture under heavy chewing forces. Additionally, the opacity required to mask the metal substrate prevents the light transmission that creates natural tooth translucency, making PFM crowns appear somewhat lifeless compared to all-ceramic alternatives.
All-Ceramic, Zirconia, and Pressed Ceramic Crowns
All-ceramic crowns represent the current state-of-the-art for anterior restorations where aesthetics are paramount. Modern ceramic systems—including lithium disilicate, feldspathic porcelain, and leucite-reinforced ceramics—achieve strength levels approaching 400 MPa while maintaining excellent light transmission and color-matching capabilities. These materials can be precisely shade-matched to adjacent teeth and demonstrate excellent biocompatibility with minimal plaque accumulation.
Zirconia crowns have revolutionized posterior crown therapy by delivering metal-like strength (900-1200 MPa) in a tooth-colored material. Zirconia’s crystalline structure provides exceptional fracture resistance while its white color eliminates the aesthetic concerns associated with metal crowns. Recent advances in zirconia processing have improved translucency, making these crowns viable for anterior applications where both strength and aesthetics matter.
Pressed ceramic systems use heat and pressure to form crowns from ceramic ingots, creating restorations with superior fit and minimal porosity compared to built-up ceramics. The pressing process eliminates many fabrication variables that can compromise crown quality, while multiple translucency levels allow customization for different aesthetic requirements. These systems particularly excel in anterior applications where precise color matching and natural translucency are essential.
The primary consideration with all-ceramic crowns involves their brittleness compared to metals. While modern ceramics achieve impressive strength, they remain susceptible to sudden fracture under extreme forces. Patients with heavy chewing habits or bruxism may require night guards to protect ceramic restorations from excessive stress.
All-Resin and Same-Day Crowns
All-resin crowns offer an economical option for patients seeking tooth-colored restorations, particularly in temporary or transitional situations. Modern composite resins achieve reasonable strength and aesthetics while allowing for easy repair if damage occurs. However, resin’s tendency to stain, wear, and degrade over time limits their longevity compared to ceramic or metal alternatives. Most resin crowns require replacement within 5-7 years, making them less cost-effective for permanent restorations.
Same-day crown technology utilizes chairside CAD/CAM (Computer-Aided Design/Computer-Aided Manufacturing) systems to design, mill, and place crowns in a single appointment. These systems—led by platforms like CEREC—use digital impressions to create crown designs that are then milled from ceramic blocks in the dental office. The entire process typically takes 2-3 hours, eliminating temporary crowns and multiple appointments while delivering immediately functional restorations.
The appeal of same-day crowns extends beyond convenience. Immediate placement preserves tooth structure that might be lost during the interim period with temporary crowns, while eliminating the variables introduced by laboratory fabrication and shipping. However, the materials available for chairside milling are currently limited compared to laboratory options, and the complexity of shade matching may not achieve the same results as laboratory-fabricated crowns for highly aesthetic cases.
Longevity, Durability, and Common Complications of Dental Crowns
Clinical research reveals that crown longevity varies significantly based on material selection, placement technique, patient habits, and maintenance practices. Large-scale studies tracking crown performance over 10-15 years show success rates ranging from 85-95%, with failure modes that often follow predictable patterns related to these variables.
Factors Affecting Longevity and Success Rates
Material choice significantly impacts crown lifespan, with gold alloys demonstrating the longest clinical track record—often exceeding 20 years—followed by well-made PFM crowns at 12-15 years. All-ceramic crowns show promising longevity data, with lithium disilicate and zirconia systems achieving 10-12 year survival rates that continue improving as techniques mature. The key factor isn’t just material strength but how well the material’s properties match the specific clinical requirements of each case.
Patient habits dramatically influence crown survival. Patients who grind or clench their teeth (bruxism) create forces that can exceed any dental material’s fatigue limit, leading to crown fracture or loosening. Similarly, habits like ice chewing, nail biting, or using teeth as tools can generate the sudden high forces that cause ceramic crowns to fracture. Research indicates that patients with parafunctional habits benefit from protective night guards and may need to avoid the most brittle crown materials.
Oral hygiene around crowned teeth requires special attention because the crown-tooth margin creates a potential site for bacterial accumulation and secondary decay. Studies show that crowns with good margin adaptation and patients with excellent oral hygiene can last decades, while poor hygiene leads to crown failure through decay of the underlying tooth structure. The cement seal at the crown margin must remain intact to prevent bacterial infiltration that compromises the tooth from within.
Regular dental monitoring proves essential for early detection of crown problems before they become symptomatic. Dentists can identify subtle changes in crown fit, early signs of wear or chipping, and gum health around crown margins during routine examinations. Early intervention—such as adjusting high spots or addressing minor chips—can extend crown life significantly compared to waiting until problems become painful or visible to patients.
Biological and Aesthetic Considerations
Gum health around crowned teeth depends heavily on crown design and margin placement. Crowns with margins placed at or slightly below the gum line tend to accumulate more plaque than those finished at the gum level, requiring more diligent home care and professional cleaning. The crown material itself affects gum response—highly polished ceramics and gold typically show less plaque accumulation than rougher surfaces, leading to better long-term gum health.
Color stability varies significantly among crown materials, with important implications for aesthetic longevity. All-ceramic and zirconia crowns maintain their color essentially permanently, while resin-based materials may stain or discolor over time, particularly with exposure to coffee, tea, or tobacco. Even small color changes can make crowns appear obvious against natural teeth, necessitating replacement for aesthetic reasons even when the crown remains functionally sound.
Biocompatibility concerns are minimal with modern crown materials, but individual sensitivities can occur. Metal allergies, while rare, most commonly involve nickel or other base metals used in some alloy systems. High-noble metal alloys (high gold content) and all-ceramic materials demonstrate excellent biocompatibility for virtually all patients. However, some patients report sensitivity to pressure or temperature changes after crown placement, usually resolving within a few weeks as the tooth adapts to its new restoration.
The aesthetic integration of crowns with natural teeth requires consideration of how materials age differently. Natural teeth gradually darken and wear over time, while ceramic crowns maintain their original color and form. This can lead to aesthetic mismatches developing years after placement, even when crowns were initially well-matched. Understanding this aging dynamic helps set realistic expectations for crown longevity, particularly in the aesthetic zone.
Technological Advances in Dental Crown Fabrication
Digital dentistry has fundamentally transformed crown fabrication from an analog process relying on physical impressions and manual techniques to a precision-engineered workflow that eliminates many traditional sources of error. These advances aren’t just improving convenience—they’re enabling crown designs and fits that surpass what was possible with conventional methods.
Digital impression systems have moved beyond simple convenience to capture anatomical details that traditional impressions often miss or distort. Modern intraoral scanners use structured light patterns or confocal imaging to create point-cloud data with accuracy measured in micrometers. This precision translates directly into better crown fit, particularly at the critical crown-tooth margin where seal integrity determines long-term success. The ability to immediately verify scan quality and rescan specific areas ensures that fabrication begins with optimal data.
CAD/CAM design software applies engineering principles to crown design in ways that were impossible with manual wax-up techniques. Software can automatically calculate optimal wall thickness for different materials, design internal surface textures that enhance cement retention, and optimize contact points with adjacent teeth. Advanced programs even simulate chewing forces to identify potential stress concentrations before fabrication begins, allowing design modifications that improve crown longevity.
3D printing is beginning to revolutionize crown fabrication, particularly for complex cases requiring custom geometries. While most crowns are still milled from solid ceramic blocks, 3D printing enables fabrication of internal frameworks with hollow designs that reduce weight while maintaining strength. This technology particularly benefits large span bridges and full-mouth reconstructions where conventional fabrication methods become prohibitively complex or expensive.
Artificial intelligence integration in crown design represents the cutting edge of current development. AI systems trained on thousands of successful crown cases can suggest optimal preparations, predict potential complications, and recommend design modifications based on patient-specific factors like bite force, tooth position, and aesthetic requirements. While still emerging, these systems promise to democratize expert-level crown design across all practitioners.
The integration of these technologies creates a digital workflow where crown design, fabrication, and placement become more predictable and precise. Digital records enable perfect remake capabilities, while process standardization reduces the technique sensitivity that historically made crown success dependent on individual practitioner skill. For patients, this translates into better-fitting crowns, reduced adjustment appointments, and more predictable long-term outcomes.
Maintenance and Care for Dental Crowns
Crowned teeth require specific care strategies that differ from natural tooth maintenance, primarily because the crown-tooth interface creates unique vulnerabilities that don’t exist with intact teeth. Understanding these requirements helps ensure that crown investments provide maximum service life while maintaining optimal oral health.
Daily hygiene around crowns focuses on the crown margins where bacteria can accumulate and potentially compromise the underlying tooth structure. Traditional flossing remains essential, but technique matters—aggressive flossing can dislodge crowns with compromised cement seals, while inadequate cleaning allows bacterial buildup. Water flossers provide excellent cleaning around crown margins and prove particularly valuable for patients with dexterity limitations or complex crown work.
Dietary considerations become important because certain foods can damage specific crown materials or challenge crown retention. Ice chewing, hard candy, and sticky foods can fracture ceramic crowns or pull off crowns with weakened cement seals. Patients with ceramic crowns benefit from cutting corn off the cob rather than biting directly, while those with any crown type should avoid using teeth as tools for opening packages or bottles.
Professional maintenance requirements may increase for patients with crowns, particularly those with multiple restorations. Dental hygienists can identify early signs of crown problems—subtle margin gaps, rough surfaces, or gum changes—that patients typically don’t notice until problems become symptomatic. Professional cleanings also address plaque accumulation in areas that home care might miss, preventing the secondary decay that represents one of the most common causes of crown failure.
Protective appliances become essential for patients with bruxism or contact sports participation. Night guards distribute grinding forces across multiple teeth rather than concentrating them on individual crowns, significantly extending crown life. Sports guards protect against sudden impact forces that can fracture even the strongest crown materials. The investment in protective appliances typically pays for itself by preventing crown damage that requires expensive replacement.
Monitoring and early intervention prove crucial for maximizing crown longevity. Patients should report any changes in bite feel, sensitivity, or crown appearance promptly, as early problems are often easily correctable while delayed treatment may require crown replacement. Regular professional examinations can detect margin deterioration, cement washout, or crown loosening before catastrophic failure occurs, often allowing simple re-cementation rather than complete crown replacement.
The key insight for crown maintenance lies in recognizing that crowns, while durable, remain artificial restorations that require ongoing attention. Unlike natural teeth that can adapt and repair minor damage, crowns depend entirely on their initial integrity and proper care for long-term success. Patients who embrace this reality and adjust their habits accordingly typically achieve crown service lives that justify the initial investment while maintaining excellent oral health around their restorations.
Modern crown therapy represents a maturation of both materials science and digital fabrication that offers patients unprecedented options for restoring damaged teeth. The evolution from one-size-fits-all approaches to sophisticated material selection based on individual needs, combined with digital workflows that enhance precision, has made crown success increasingly predictable. Yet the fundamentals remain unchanged—proper diagnosis, skilled preparation, appropriate material selection, and committed maintenance determine long-term outcomes. As dental technology continues advancing, the goal stays constant: preserving natural tooth structure while restoring full function and aesthetic integration that serves patients for decades. The crown options available today make this goal achievable for virtually every clinical situation, provided the treatment approach matches the patient’s specific needs and commitment to ongoing care.