Health Benefits of Dental Bridges and How They Work
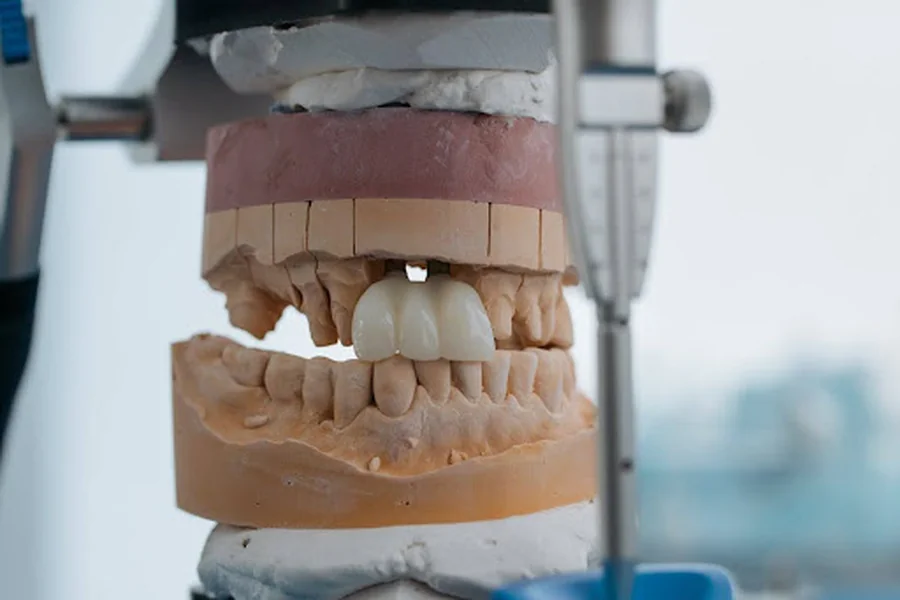
When 178 million Americans are missing at least one tooth, and 40 million have lost all their teeth, the ripple effects extend far beyond cosmetics. Recent dental research shows that people with missing teeth face a 32% higher risk of cognitive decline and experience an average 15% reduction in chewing efficiency—consequences that compound over time. What’s particularly striking is how quickly adjacent teeth begin shifting into empty spaces, often creating bite problems within just six months of tooth loss.
The traditional approach of “waiting to see what happens” after tooth loss has given way to a more proactive understanding of oral health’s systemic impact. Dental professionals now recognize that replacing missing teeth isn’t just about restoring smiles—it’s about preserving the structural integrity of your entire mouth and supporting long-term health outcomes. Modern custom bridge restorations in Cary, NC have evolved to address these challenges more effectively than ever before, offering a fixed solution that works with your natural bite mechanics.
Here’s what the latest research reveals about how dental bridges protect not just individual teeth, but your overall oral health ecosystem—and why timing matters more than most people realize.
What Are Dental Bridges and Who Is Eligible?
Definition and Purpose of Dental Bridges
A dental bridge literally bridges the gap where one or more teeth are missing, using adjacent teeth as anchors to support a replacement tooth (called a pontic). Think of it as creating a three-unit structure: two crowns on either side of the gap that hold a replacement tooth in the middle. This fixed restoration becomes part of your mouth’s architecture, unlike removable dentures that sit on top of your gums.
The engineering behind bridges relies on load distribution—spreading the forces of chewing across multiple teeth rather than concentrating stress on a single point. When you bite down, the pressure gets distributed through the bridge structure to the supporting teeth, which then transfer that force to your jawbone through their roots. This biomechanical approach helps maintain the natural function your mouth was designed for.
Modern bridge construction has evolved significantly since the 1970s. Today’s materials can withstand bite forces up to 200 pounds per square inch while maintaining a natural appearance that’s virtually indistinguishable from your original teeth. The key innovation lies in how bridges integrate with your existing oral structures rather than simply replacing what’s missing.
Criteria for Dental Bridge Candidacy
Not everyone qualifies for a traditional dental bridge, and understanding the criteria helps explain why bridges work so effectively when properly applied. The supporting teeth (called abutments) must have sufficient structural integrity to handle the additional load. Dentists evaluate bone density, gum health, and the overall condition of adjacent teeth before recommending a bridge.
Healthy adjacent teeth represent the primary requirement. If neighboring teeth have extensive decay, large fillings, or periodontal disease, they may not provide adequate support. However, teeth with minor issues can often be restored first, then used as bridge abutments. The evaluation process includes X-rays to assess root structure and bone levels around potential supporting teeth.
Age and oral hygiene habits also factor into candidacy decisions. Younger patients with good oral care routines typically experience better long-term outcomes, but age alone doesn’t disqualify someone from bridge treatment. What matters more is the patient’s ability to maintain proper oral hygiene around the bridge structure, which requires specific techniques for cleaning under the pontic.
How Do Dental Bridges Restore Oral Function?
Installation Process Overview
Bridge installation requires precision planning that begins weeks before the actual procedure. Your dentist creates a treatment plan based on impressions, X-rays, and bite analysis to ensure the finished bridge will integrate seamlessly with your natural chewing patterns. This planning phase often reveals bite irregularities that can be corrected during the bridge placement process.
The procedure itself typically spans two appointments separated by 2-3 weeks. During the first visit, the abutment teeth are prepared by removing a thin layer of enamel to accommodate the crowns that will support the bridge. Local anesthesia ensures comfort throughout this process, and a temporary bridge protects the prepared teeth while your permanent bridge is fabricated in a dental laboratory.
Precision fitting occurs during the second appointment, when your dentist checks the bridge’s fit, bite alignment, and appearance before permanently cementing it in place. Modern dental adhesives create a bond stronger than the original tooth structure, essentially making the bridge a permanent part of your mouth’s architecture.
Materials Used in Dental Bridge Construction
Today’s dental bridges utilize materials that balance strength, aesthetics, and biocompatibility. Porcelain-fused-to-metal (PFM) bridges combine a metal substructure for strength with a porcelain outer layer for natural appearance. The metal core—typically gold alloy, palladium, or base metals—provides durability while the porcelain allows for precise color matching to your existing teeth.
All-ceramic bridges, made from materials like zirconia or lithium disilicate, offer superior aesthetics and work especially well for front teeth where appearance matters most. These materials reflect light similarly to natural tooth enamel, creating a more lifelike appearance under different lighting conditions. Advanced ceramics also resist staining better than older materials, maintaining their appearance over time.
The choice of material depends on the bridge’s location, your bite forces, and aesthetic requirements. Back teeth that handle heavy chewing typically benefit from the strength of PFM construction, while front teeth often use all-ceramic materials for optimal appearance. Your dentist considers these factors alongside your budget and long-term oral health goals when selecting bridge materials.
Types and Variations of Dental Bridges
Traditional and Cantilever Bridges
Traditional bridges represent the most common design, using crowns on adjacent teeth to support one or more replacement teeth. This approach works best when healthy teeth exist on both sides of the gap, providing balanced support for the bridge structure. The biomechanics mirror how natural teeth share chewing forces, creating a stable foundation that can last decades with proper care.
Cantilever bridges offer a solution when only one adjacent tooth is available for support, though their applications are more limited. Like a diving board anchored at one end, cantilever bridges extend from a single supporting tooth to replace a missing adjacent tooth. This design requires extra care in bite adjustment since all forces concentrate on the single abutment tooth.
Modern engineering has improved cantilever bridge success rates through better materials and design modifications. Dentists now use computer modeling to optimize the bridge structure, ensuring forces distribute as evenly as possible through the supporting tooth. However, cantilever bridges work best for replacing single front teeth where chewing forces are lighter.
Maryland and Implant-Supported Bridges
Maryland bridges (also called resin-bonded bridges) take a conservative approach by bonding to the backs of adjacent teeth rather than requiring full crown preparation. Metal or ceramic wings attach to the inner surfaces of neighboring teeth, supporting a replacement tooth without significantly altering healthy tooth structure. This technique works particularly well for replacing front teeth in younger patients.
The trade-off with Maryland bridges involves durability—they’re more prone to debonding than traditional bridges and typically don’t handle heavy chewing forces as well. However, for patients who want to preserve maximum natural tooth structure while replacing a missing tooth, Maryland bridges provide an appealing middle ground between temporary solutions and more invasive procedures.
Implant-supported bridges represent the most advanced option, using dental implants rather than natural teeth as anchors. This approach preserves adjacent teeth entirely while providing the strongest possible foundation. When replacing multiple teeth, implant-supported bridges can span larger gaps using fewer implants than would be needed for individual implant crowns, making them cost-effective for extensive tooth replacement.
Key Health Benefits of Dental Bridges
Restoring Chewing Ability and Bite Force Distribution
The immediate impact of missing teeth on your ability to chew efficiently often surprises patients. Research indicates that each missing tooth reduces chewing efficiency by approximately 10%, and the effects compound as you unconsciously compensate by favoring one side of your mouth. This compensation pattern leads to uneven wear on remaining teeth and can trigger jaw joint problems over time.
Dental bridges restore your natural bite mechanics by providing stable surfaces for effective chewing. Unlike removable appliances that can shift during eating, bridges remain fixed in place, allowing you to apply normal chewing forces without worry. This stability means you can return to eating foods you may have avoided since tooth loss, improving both nutrition and quality of life.
The biomechanical benefits extend beyond simple replacement. Bridges help redistribute chewing forces across multiple teeth, preventing the overloading that occurs when adjacent teeth must handle extra work. This load sharing protects your remaining natural teeth from excessive wear and reduces the risk of stress fractures that can occur when teeth must handle forces beyond their normal capacity.
Maintaining Facial Structure and Preventing Teeth Shifting
Your teeth act as internal scaffolding for your facial muscles and lips, providing support that maintains your natural facial height and profile. When teeth are missing, especially back teeth that provide crucial vertical support, facial muscles can begin to sag inward, creating a prematurely aged appearance. This effect becomes more pronounced over time as the lack of support allows facial tissues to collapse.
Dental bridges maintain facial vertical dimension by preserving the proper spacing between your upper and lower jaws. This support keeps your facial muscles positioned correctly, preventing the sunken-cheek appearance that can develop after tooth loss. The effect is particularly noticeable around the lips and cheeks, which rely on underlying tooth structure for proper positioning.
Perhaps more immediately concerning is how quickly adjacent teeth begin moving into empty spaces. Without the lateral pressure from neighboring teeth, your remaining teeth start tilting and shifting within just a few months of tooth loss. This movement creates bite problems, makes cleaning more difficult, and can eventually compromise the stability of additional teeth. Bridges prevent this shifting by maintaining proper spacing and providing the lateral support your teeth need to stay properly aligned.
Improving Speech Clarity and Oral Hygiene
The position of your teeth plays a crucial role in speech production, particularly for sounds that require tongue placement against teeth or precise airflow control. Missing front teeth obviously affect sounds like “th” and “s,” but even missing back teeth can impact speech clarity by changing how your tongue moves within your mouth or altering the resonance of your oral cavity.
Bridges restore the natural landmarks your tongue relies on for clear speech production. Unlike removable appliances that can affect speech by covering portions of your palate or shifting during talking, bridges provide fixed reference points that allow your tongue to function normally. Most patients find their speech returns to normal within days of bridge placement, once they adjust to the restored tooth positions.
From a hygiene perspective, bridges create surfaces that are easier to clean than the irregular spaces left by missing teeth. Food particles and bacteria tend to collect in empty tooth sockets and around tilted adjacent teeth, creating areas that are difficult to clean effectively. While bridges require specific cleaning techniques under the pontic area, they eliminate the hard-to-reach spaces that commonly develop problems after tooth loss.
Reducing Risk of Gum Disease and Bone Loss
The bone that supports your teeth requires stimulation from chewing forces to maintain its density and volume. When teeth are missing, the underlying bone begins resorbing—essentially dissolving away—because it no longer receives the mechanical stimulation that signals your body to maintain that tissue. This bone loss can accelerate the aging process and complicate future dental treatment options.
Bridges help preserve bone by transmitting chewing forces through the supporting teeth to the surrounding bone tissue. While they don’t provide the same direct stimulation as tooth roots, they maintain much of the mechanical loading that helps preserve bone density. This is particularly important for maintaining the proper support for adjacent teeth and preserving facial structure over time.
The gum health benefits come from eliminating the hard-to-clean areas that develop around missing teeth. Empty sockets tend to collect food debris and bacteria, creating chronic inflammation that can spread to adjacent teeth. Bridges provide smooth, cleansable surfaces that support better oral hygiene practices and reduce the bacterial accumulation that leads to periodontal disease.
Dental Bridges Compared With Dentures and Implants
Durability and Comfort Differences
When comparing tooth replacement options, the stability and longevity differences become apparent within the first few weeks of use. Dental bridges offer fixed stability that eliminates the movement and adjustment issues common with removable dentures. Patients report being able to eat, speak, and function normally almost immediately after bridge placement, whereas denture wearers often require months of adjustment and may never achieve the same level of function.
Partial dentures, while less expensive initially, create unique challenges that bridges avoid entirely. The metal clasps used to secure partial dentures can weaken supporting teeth over time through constant flexing forces. Additionally, the plastic and metal components of dentures can harbor bacteria more readily than the smooth ceramic surfaces of bridges, potentially increasing the risk of oral infections.
The comfort factor extends beyond initial adaptation. Bridges don’t require adhesives, daily removal for cleaning, or special storage considerations. They function like natural teeth, requiring only normal brushing and flossing with some modification for cleaning under the pontic. This simplicity translates to better long-term compliance with oral hygiene routines and fewer maintenance-related complications.
Functional and Cosmetic Advantages
From a functional standpoint, bridges restore approximately 90-95% of normal chewing efficiency, compared to 60-70% for well-fitted dentures and nearly 100% for implant-supported restorations. This difference impacts not just what you can eat, but how effectively your body can extract nutrients from food during the digestive process. Improved chewing efficiency contributes to better overall health outcomes, particularly for older adults who may already face nutritional challenges.
The cosmetic advantages of bridges stem from their fixed nature and custom fabrication. Unlike dentures that can create artificial-looking bulk in the mouth or visible metal clasps, bridges blend seamlessly with your natural teeth. Modern ceramics can be precisely matched to your existing tooth color and translucency, creating results that are virtually indistinguishable from natural teeth.
Bridge aesthetics also remain stable over time. While dentures may shift position or wear unevenly, bridges maintain their original appearance and function throughout their lifespan. The only visible change typically occurs after many years when normal gum recession around the bridge margins may create small spaces—an issue that can usually be addressed with minor adjustments.
Bone Preservation and Long-Term Health Impact
The long-term health implications of different tooth replacement options become more apparent over decades rather than years. While implants provide the best bone preservation by directly stimulating the jawbone through artificial roots, bridges offer significant advantages over removable options by maintaining many of the forces that help preserve facial structure and bone density.
Denture wearers experience accelerated bone loss because the appliance rests on top of the gums rather than providing the deep stimulation that tooth roots deliver to supporting bone. This progressive bone loss requires periodic denture relines or replacements and can eventually compromise facial support. Bridges, by contrast, maintain stimulation to the bone around the supporting teeth, helping preserve the structural foundation of your mouth.
The systemic health benefits of proper tooth replacement extend beyond oral health. Research has linked tooth loss to increased risks of cardiovascular disease, diabetes complications, and cognitive decline—associations that may relate to both nutritional impacts from poor chewing function and inflammatory processes from oral health problems. By maintaining proper oral function and supporting better oral hygiene, bridges may contribute to broader health benefits that compound over time.
Maintenance and Longevity of Dental Bridges
Daily Care Tips for Prolonging Bridge Life
Effective bridge maintenance requires adapting your daily oral hygiene routine to address the unique cleaning challenges created by the bridge structure. The area under the pontic—where the replacement tooth meets the gum—requires special attention since normal brushing can’t reach this space effectively. Floss threaders or water flossers become essential tools for removing bacteria and food particles from under the bridge.
The technique for cleaning under bridges involves threading floss beneath the pontic and gently moving it back and forth to remove debris. This process should be performed daily, preferably before bedtime when bacteria have more opportunity to accumulate overnight. Water flossers provide an alternative that many patients find easier to use consistently, though they shouldn’t completely replace traditional flossing for areas around natural teeth.
Regular brushing remains important for the crowned supporting teeth, which can still develop decay at the gum line where the crown meets the natural tooth. Using fluoride toothpaste helps protect these vulnerable areas, and some patients benefit from prescription-strength fluoride treatments to provide extra protection for the supporting teeth that now bear additional load.
Common Causes of Dental Bridge Failure
Understanding why bridges fail helps patients avoid the behaviors and conditions that compromise their longevity. Decay at the crown margins represents the most common cause of bridge failure, typically developing where the crown edges meet the natural tooth structure. This occurs when oral hygiene around the bridge becomes inadequate, allowing bacteria to accumulate and produce acids that dissolve tooth structure.
Mechanical failure can result from excessive forces, often related to grinding or clenching habits that weren’t present when the bridge was originally designed. Night guards may be recommended for patients who develop these habits after bridge placement, as the concentrated forces can fracture ceramic materials or loosen the cement bond holding the bridge in place.
Periodontal disease around the supporting teeth poses another significant risk factor. If the gums and bone around the abutment teeth become compromised, the foundation supporting the bridge weakens. This emphasizes the importance of maintaining excellent oral hygiene not just around the bridge itself, but throughout the entire mouth to preserve the health of the supporting structures.
Average Longevity and Recurring Procedures
Well-maintained dental bridges typically last 10-15 years, with many exceeding this timeframe when supported by excellent oral hygiene and regular professional care. Factors influencing longevity include the patient’s bite forces, oral hygiene compliance, the health of supporting teeth at placement, and the bridge’s location in the mouth. Back teeth that handle heavier chewing forces may experience shorter lifespans than front tooth bridges.
When bridges do require replacement, the process often involves evaluating the supporting teeth to determine if they remain suitable for another bridge. If the abutment teeth have remained healthy, a new bridge can typically be fabricated using the same support structure. However, if decay or other problems have compromised the supporting teeth, alternative treatment approaches may be necessary.
The timing of bridge replacement usually becomes apparent during routine dental examinations before patients experience problems. Regular X-rays can detect decay or bone changes around supporting teeth, while clinical examination reveals changes in fit or function. This proactive approach allows for planned replacement rather than emergency treatment when bridges fail unexpectedly.
Advances and Future Trends in Dental Bridge Technology
Innovations in Materials and Design
Recent advances in dental ceramics have produced materials that surpass the strength and aesthetics of earlier bridge options while requiring less invasive tooth preparation. Zirconia-based ceramics now offer flexural strengths exceeding 1,000 MPa while maintaining translucency that rivals natural tooth enamel. These materials resist chipping and wear while providing superior stain resistance compared to traditional ceramics.
Computer-aided design and manufacturing (CAD/CAM) technology has revolutionized bridge fabrication, allowing for more precise fit and improved aesthetics. Digital impressions eliminate the discomfort of traditional impression materials while providing more accurate data for bridge construction. This precision translates to better-fitting bridges that require fewer adjustments and provide improved long-term comfort.
Adhesive technology has also evolved significantly, with new bonding agents creating stronger, more durable connections between bridges and natural teeth. Modern adhesives can form chemical bonds with both tooth structure and ceramic materials, creating integrated systems that function more like natural teeth than traditional mechanical attachments.
Minimally Invasive Techniques and Clinical Success Factors
The trend toward conservative dentistry has influenced bridge design, with techniques that preserve more natural tooth structure while maintaining strength and longevity. Ultra-thin ceramic materials allow for bridges that require minimal tooth reduction, preserving healthy tooth structure that contributes to long-term success.
Digital workflow integration has streamlined the bridge process, reducing treatment time and improving patient comfort. Same-day bridge options are becoming available for certain cases, though traditional multi-visit protocols remain the gold standard for complex cases requiring precise bite adjustment and optimal aesthetics.
Clinical success factors now emphasize the importance of comprehensive treatment planning that considers the patient’s entire oral health ecosystem rather than just replacing missing teeth. This holistic approach includes evaluating and treating periodontal disease, addressing bite irregularities, and ensuring adequate oral hygiene skills before bridge placement.
Emerging Trends in Bridge Development
The integration of biomimetic principles in bridge design focuses on replicating the natural stress distribution patterns of intact teeth. New bridge designs incorporate flexible connectors and shock-absorbing elements that better mimic how natural teeth respond to chewing forces, potentially extending bridge lifespan and reducing complications.
3D printing technology is beginning to influence bridge fabrication, offering the potential for more complex internal structures that optimize strength while reducing weight. These manufacturing advances may allow for bridge designs that weren’t possible with traditional fabrication methods, potentially improving both function and durability.
Research into bioactive materials that can stimulate remineralization of adjacent tooth structure represents an exciting frontier. These materials could potentially strengthen the supporting teeth over time rather than simply replacing missing tooth structure, fundamentally changing how we think about the long-term interaction between bridges and natural teeth.
As digital dentistry continues to evolve, the future likely holds even more precise, durable, and biocompatible bridge options that provide patients with tooth replacement solutions that truly function like natural teeth. The convergence of advanced materials science, digital manufacturing, and improved understanding of oral biomechanics promises bridge treatments that offer better outcomes with less invasive procedures than ever before possible.